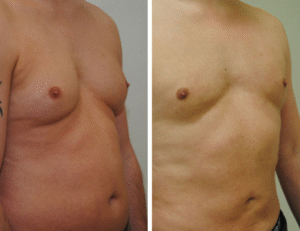
Gynecomastia surgery before a wedding in Gurgaon is among the most requested pre-wedding procedures among grooms at Artemis Hospital — and the least discussed openly. Most grooms have managed the same concern for years: avoiding fitted shirts, choosing thicker fabrics, positioning themselves carefully in photographs. The wedding makes that quiet management impossible.
The sherwani is the catalyst for many grooms. A lehenga blouse accommodates breast fullness by design. A sherwani does not. Its structured front and tailored silhouette are designed for a flat, masculine chest — any fullness in the chest tissue, particularly at the nipple area, creates a visible contour disruption that tailoring alone cannot address.
Book a groom’s consultation with Dr. Pradeep Kumar Singh at Artemis Hospital, Gurugram, or call +91 82879 23924 to assess your gynecomastia grade and plan your pre-wedding timeline.
Why Gynecomastia Develops — and Why Exercise Does Not Fix It
Gynecomastia is the clinical term for the development of glandular breast tissue in males. It is not the same as chest fat accumulation — a distinction that matters practically, because the two conditions require different treatments and the glandular component of gynecomastia does not respond to exercise or fat loss.
The most common causes in the age group of grooms presenting for pre-wedding consultations in Gurgaon include:
- Hormonal imbalance during puberty: Gynecomastia affects an estimated 50 to 70 per cent of adolescent males during puberty, driven by a temporary oestrogen-testosterone imbalance. In most cases, it resolves naturally; in approximately 25 per cent of cases, the glandular tissue remains permanently, which is why many men in their twenties and thirties carry it despite low body fat.
- Anabolic steroid use: Anabolic steroids convert to oestrogen through aromatisation, stimulating glandular tissue growth. This form tends to be rapid in onset and consistently glandular.
- Idiopathic causes: In a significant proportion of adult cases, no identifiable hormonal or pharmacological cause is found. The tissue is present and permanent without a diagnosable trigger.
The critical point for grooms who have tried gym training, dietary changes, and targeted chest exercises without result: if the fullness in your chest is caused by glandular tissue — and not adipose tissue alone — no amount of exercise will remove it. Male breast reduction surgery is the only effective treatment for the glandular component of gynecomastia.
Gynecomastia Grades and What They Mean for Your Pre-Wedding Timeline
Not all gynecomastia is the same in severity, and the grade of your gynecomastia directly determines both the surgical approach and the recovery timeline available before your wedding. The Simon classification system, widely used by plastic surgeons in India, divides gynecomastia into four grades:
| Grade | What It Looks Like | Surgical Approach | Pre-Wedding Window |
| Grade I | Minor enlargement, no excess skin | Glandular excision ± VASER liposuction | 3–4 months |
| Grade IIa | Moderate enlargement, no skin excess | Glandular excision + VASER liposuction | 3–4 months |
| Grade IIb | Moderate enlargement, minor skin excess | Excision + liposuction + minor skin reduction | 4–5 months |
| Grade III | Marked enlargement, significant skin excess | Mastectomy with skin excision | 5–6 months minimum |
The grade assessment is made during the clinical consultation. Dr. Pradeep Kumar Singh evaluates both the glandular and fat components, determines the appropriate surgical approach, and maps the plan to the available pre-wedding timeline.
VASER Liposuction vs Glandular Excision: Which Approach Is Right for You
The two primary surgical techniques used in male breast reduction surgery are VASER-assisted liposuction and direct glandular excision. In many cases, both are used together, and understanding the difference helps grooms know what to expect from their procedure.
- VASER liposuction: VASER uses ultrasound energy to emulsify fat before removal, producing smooth chest contouring with minimal bruising. It is highly effective for the adipose component but does not remove glandular tissue — the firm disc beneath the nipple that defines true gynecomastia. Where this glandular component is significant, VASER liposuction alone will not produce a flat chest.
- Direct glandular excision: A small periareolar incision at the areola border allows direct removal of the glandular disc — the definitive treatment for the glandular component. The incision (typically 2–3 cm) sits at the natural colour boundary of the areola and heals to a faint line not visible through clothing.
- Combined approach: Most cases at Artemis Hospital use both: VASER liposuction for fat and chest contouring, followed by periareolar glandular excision for the firm disc. The combined approach produces the flattest, most masculine chest contour and is standard for Grade IIa and IIb presentations.
Week-by-Week Recovery: What a Groom Needs to Plan For
Gynecomastia surgery recovery is considerably more manageable than most grooms anticipate — and significantly shorter than the recovery timelines for procedures brides typically plan. Here is what the recovery looks like in practice:
- Days 1–3: Drain removal (if used) and transition to a compression vest worn continuously. The chest will feel tight and tender. Most patients manage discomfort with standard pain medication. Activity is restricted to gentle walking.
- Week 2: Most grooms return to desk-based work. The compression vest is worn continuously for the first three to four weeks. Driving is possible once pain medication is no longer needed. The chest appears swollen and firm — this is normal and expected at this stage.
- Week 3–4: Visible swelling begins to reduce noticeably. The chest starts to look flatter. The compression vest transitions to being worn during the day only. Light activity resumes, but chest exercises and heavy lifting remain restricted.
- Month 2: Approximately 70 per cent of swelling has resolved. Most grooms can wear a fitted shirt without visible chest fullness by this point. Sherwani fittings at month 2 give a reasonable — though not final — measurement.
- Month 3: The final chest contour is visible for 90 per cent of cases. The periareolar scar is present but fades to a faint line that sits at the areola border. A sherwani fitting at three months provides an accurate measurement for the tailored garment.
Grooms from Magnolias, M3M Golf Estate, Golf Course Road, Sector 56, Sushant Lok, Nirvana Country, Defence Colony, Chanakyapuri, Jor Bagh, and Greater Kailash who had gynecomastia surgery three to four months before their wedding consistently report that month three was the point at which they felt ready — and that the sherwani fitting at that stage gave a measurement they were comfortable with.
Choosing the Right Gynecomastia Surgeon in Gurgaon for Pre-Wedding Surgery
Pre-wedding gynecomastia surgery has a specific performance requirement that routine cases do not: the result must be settled and visible by a fixed date, and it must look natural under the tailored, structured front of a sherwani. This requires a plastic surgeon who understands not only the surgical technique but also the grading assessment that determines whether the pre-wedding timeline is genuinely safe for the patient’s specific case.
Dr. Pradeep Kumar Singh — MCh in Plastic Surgery, SMS Medical College, Jaipur; Fellowship from St Louis Hospital, Paris; APSI member — performs gynecomastia surgery across all grades at Artemis Hospital, Sector 51, Gurugram (JCI and NABH-accredited). His assessment includes clinical grading, tissue composition evaluation, and an explicit discussion of whether the wedding date allows the correct approach.
Grooms from Ardee City, Palam Vihar, Sector 42, MG Road, Golf Course Extension, Anand Niketan, Vasant Vihar, Haus Khas, Shanti Niketan, Green Park, Gulmohar Park, and South Extension who consulted Dr. Pradeep Kumar Singh report that the clarity of the grade assessment and the honesty of the timeline conversation distinguished it from consultations elsewhere.
Frequently Asked Questions
How long before my wedding should I have gynecomastia surgery?
Grade I and IIa — the most common presentation — require three to four months for a settled result. Grade IIb cases need four to five months. Grade III, involving significant skin excess, needs a minimum of five to six months. These timelines reflect when swelling has resolved enough for the sherwani to be fitted accurately, not simply when the patient is mobile.
Will my gynecomastia come back after surgery?
Gynecomastia surgery permanently removes the glandular tissue. Once excised, it does not regenerate. If the hormonal cause is not addressed — for example, anabolic steroid use continues — residual tissue can be stimulated to enlarge. For most grooms with idiopathic or pubertal gynecomastia, the result is permanent provided weight remains stable.
Can gynecomastia surgery be done under local anaesthesia?
Minor Grade I cases involving primarily liposuction can sometimes be done under local anaesthesia with sedation. Combined procedures — the majority of cases — are performed under general anaesthesia at Artemis Hospital, allowing the surgeon to work with precision across a fully relaxed chest.
Will the scar from gynecomastia surgery be visible in my sherwani?
The periareolar incision sits at the natural colour boundary of the areola. By three months, the scar has faded to a thin line at the areola border, not visible through clothing and not apparent in close-range photography. Full scar maturation takes six to twelve months.
What if I have pseudogynecomastia — chest fat without glandular tissue?
Pseudogynecomastia is chest fullness from fat accumulation, not glandular tissue. VASER liposuction alone is highly effective for this presentation, with a somewhat faster recovery than combined excision cases. The distinction is made during clinical assessment — Dr. Pradeep Kumar Singh evaluates both components and recommends the technique based on which is the primary contributor.
Can I combine gynecomastia surgery with liposuction elsewhere?
Yes, in many cases. Grooms who want to address the chest alongside flanks, abdomen, or chin fat can combine liposuction surgery of adjacent areas with gynecomastia surgery in a single procedure. The decision to combine depends on anaesthesia duration, the patient’s overall health, and the recovery requirements. Combined procedures are appropriate for many patients — Dr. Pradeep Kumar Singh assesses suitability individually rather than applying a blanket policy.
Your Sherwani Should Fit the Way It Was Designed to Fit
Every sherwani is cut for a flat, masculine chest. Gynecomastia surgery planned at the right time produces the chest that the garment was designed for. The procedure takes two to three hours. The confidence it delivers on the wedding day lasts considerably longer.
Book now or call +91 82879 23924 to schedule your gynecomastia assessment with Dr. Pradeep Kumar Singh at Artemis Hospital.
Or visit Artemis Hospital, Sector 51, Gurugram, Haryana 122001.
Read verified patient reviews at Dr. Pradeep Kumar Singh on Google.
Dr. Pradeep Kumar Singh — MCh Plastic Surgery, Fellowship Paris, APSI Member — Head of Plastic Surgery, Artemis Hospital, Sector 51, Gurugram.