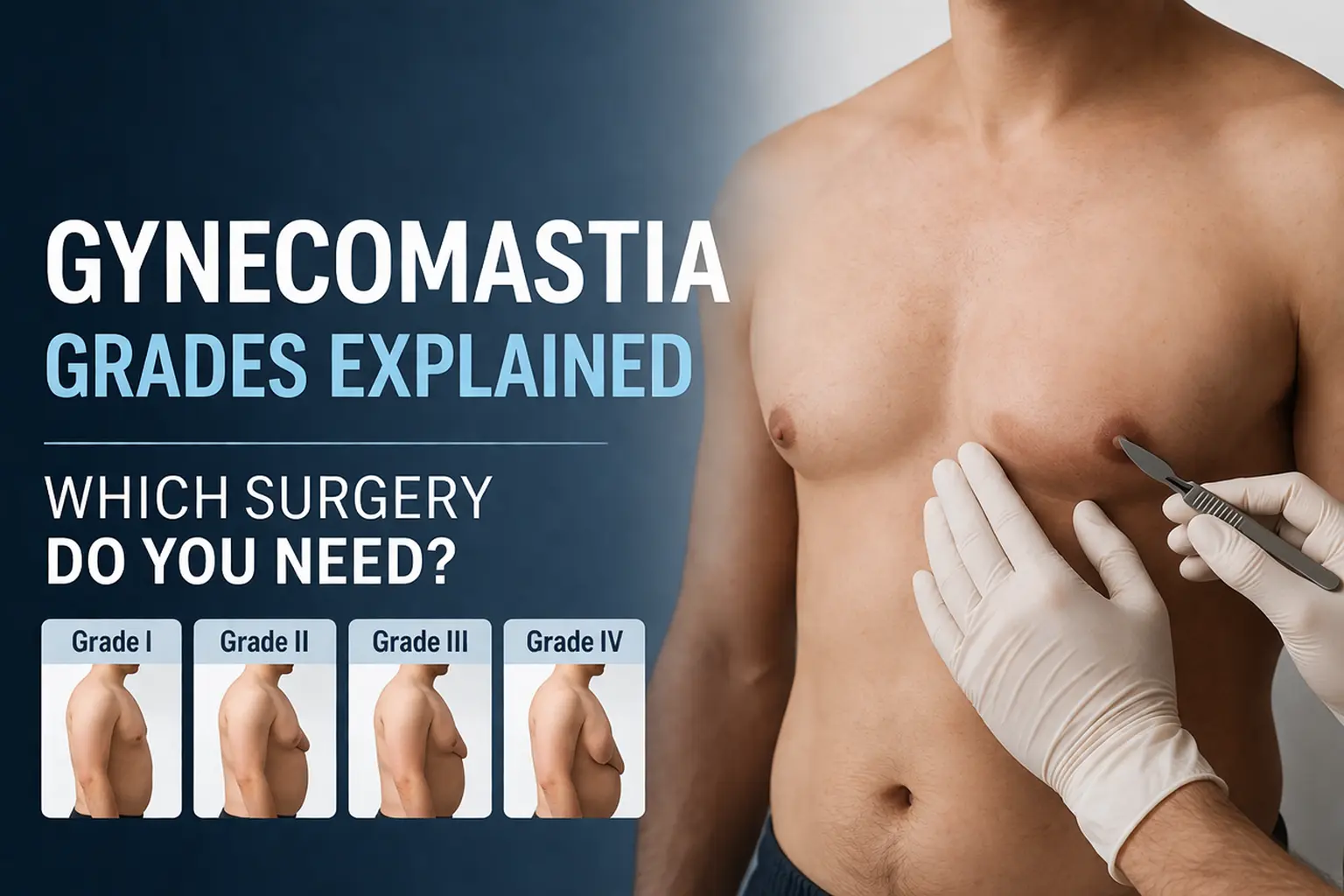
Gynecomastia grades determine everything about your surgery — the technique, incision size, recovery timeline, and final result. Two men describing the same problem may have conditions at opposite ends of the severity spectrum requiring entirely different surgical approaches. Understanding where you sit on that spectrum is the single most important output of a gynecomastia consultation — and this guide helps you arrive at that question already partially answered.
The vast majority of cases presenting at plastic surgery clinics in Gurgaon fall into Grades I and II — cases where the surgery is straightforward, and recovery is manageable. A smaller proportion involves Grade III, which requires a more involved approach. Understanding which grade applies determines the surgeon, the procedure, and the realistic outcome.
Book a gynecomastia assessment with Dr. Pradeep Kumar Singh at Artemis Hospital, Gurugram, or call +91 82879 23924 to have your grade assessed and your surgical plan outlined.
Glandular Gynecomastia vs Pseudogynecomastia: The Distinction That Changes Your Treatment
Before discussing grades, a fundamental distinction must be established: true gynecomastia and pseudogynecomastia are different conditions that require different treatments, and confusing the two is one of the most common reasons men pursue the wrong solution for years before getting an accurate diagnosis.
True gynecomastia involves glandular breast tissue development — firm, rubbery, located directly beneath the nipple. It does not respond to diet or exercise because it is not fat. No supplement, hormone therapy, or fat loss programme eliminates established glandular tissue. Surgical excision is the only effective treatment.
Pseudogynecomastia is chest fullness caused by fat accumulation rather than glandular tissue — softer, more diffuse, without a firm central disc. It responds to weight loss, and liposuction surgery alone is appropriate when fat is the primary contributor.
Many men have a mixed presentation — glandular tissue beneath the nipple alongside chest fat — requiring a combined surgical approach. The grade assessment determines the proportion of each component.
The Simon Classification: Four Grades, Four Different Surgical Solutions
The Simon classification divides gynecomastia into four grades based on the degree of breast tissue enlargement and the presence or absence of skin excess — the two variables that most directly determine surgical approach.
Grade I Gynecomastia: Minor Enlargement, No Skin Excess
Grade I is the mildest presentation — a small, palpable, firm disc behind the nipple with minor areola puffiness in certain lighting. No significant overall chest enlargement. No skin excess.
Grade I most commonly represents pubertal gynecomastia that did not fully resolve. The primary complaint is nipple prominence or puffy nipple appearance rather than overall chest size.
- Surgical approach: Glandular excision through a small periareolar incision (2–3 cm). Minor VASER liposuction may be added to refine the surrounding transition. Procedure: 45–60 minutes under general anaesthesia.
- Recovery: Swelling resolves in six to eight weeks. Compression vest for three to four weeks. Return to work within one to two weeks. Final result in two to three months.
- Scar: Small arc at the areola border (2–3 cm), fading to near-invisible within three to six months.
Grade IIa Gynecomastia: Moderate Enlargement, No Skin Excess
Grade IIa represents moderate breast tissue development with no skin excess. The chest shows visible fullness in fitted clothing, but the skin remains tight and does not fold when leaning forward.
This is the most common grade presenting for male breast reduction surgery in Gurgaon. Men with Grade IIa are typically aware of it daily, choosing clothing to conceal chest fullness and avoiding situations where the chest is visible.
- Surgical approach: VASER liposuction for the fat component combined with periareolar glandular excision (2–4 cm incision). Both performed the same procedure under general anaesthesia.
- Recovery: Compression vest for four weeks. Swelling subsides substantially by month two. The final chest contour is visible at three months.
Grade IIb Gynecomastia: Moderate Enlargement With Minor Skin Excess
Grade IIb has the tissue characteristics of Grade IIa with the addition of minor skin excess — slight looseness when leaning forward, or a subtle lower-chest droop not apparent when standing. This skin excess must be addressed to prevent residual looseness after tissue removal.
- Surgical approach: VASER liposuction, glandular excision, and a circumareolar skin reduction — removing a small skin ring around the areola and repositioning it to prevent a large or puffy appearance after tissue removal.
- Recovery: Slightly longer than Grade IIa due to additional skin work. The full result is visible at three to four months. Compression vest for four to six weeks.
Grade III Gynecomastia: Marked Enlargement With Significant Skin Excess
Grade III involves breast enlargement resembling a female breast, with significant skin excess visible at rest, not just on leaning forward. Circumareolar reduction alone is insufficient.
Grade III is less common and more frequently associated with significant weight gain and loss, long-term steroid use, or hormonal conditions. The approach is more involved, and recovery takes longer.
- Surgical approach: Subcutaneous mastectomy with skin excision. In severe cases, nipple and areola repositioning ensures natural placement after tissue removal.
- Recovery: Five to six months for full settling. A compression garment for six to eight weeks. Scars more extensive than lower grades, fading substantially over twelve months.
Quick Self-Assessment: Which Grade Are You Most Likely?
This is a guide to help you arrive at a consultation with a clearer sense of your presentation — not a substitute for clinical assessment.
| What You Notice | Most Likely Grade | Typical Surgical Approach |
| Small firm lump behind nipple, slight puffiness visible in mirror | Grade I | Glandular excision, often with minor VASER liposuction |
| Noticeable chest fullness in fitted shirts, firm lump behind nipple | Grade IIa | Combined VASER liposuction + glandular excision |
| Visible chest enlargement, mild skin looseness when leaning forward | Grade IIb | VASER + excision + circumareolar skin reduction |
| Significant chest enlargement resembling female breast, obvious skin excess | Grade III | Mastectomy with skin excision, possible nipple repositioning |
| Chest fullness that reduces significantly with weight loss, no firm lump | Pseudogynecomastia | VASER liposuction alone (no gland to excise) |
What Happens During a Gynecomastia Assessment at Artemis Hospital
A gynecomastia assessment with Dr. Pradeep Kumar Singh is a clinical examination, not a preliminary conversation. The assessment includes:
- Physical palpation: The glandular disc is identified by feel — size, firmness, and position relative to the areola. This distinguishes true gynecomastia from pseudogynecomastia and determines the glandular component.
- Tissue proportion evaluation: Determines whether VASER alone is appropriate or whether glandular excision is required.
- Skin elasticity assessment: Skin excess and elasticity determine whether circumareolar reduction or more extensive skin excision is needed.
- Hormonal cause screening: For new or rapidly developing gynecomastia, hormone blood tests may be recommended before planning surgery to rule out an active cause requiring treatment first.
Patients from DLF Phase 2, Sector 56, Golf Course Road, Magnolias, Sushant Lok, Greater Kailash, Defence Colony, Vasant Vihar, Haus Khas, Jor Bagh, Green Park, and MG Road who have undergone this assessment at Artemis Hospital report that the grade-specific surgical plan was significantly more useful than general information from online sources.
Why Grade-Specific Expertise Matters in Gynecomastia Surgery
Gynecomastia surgery is not a single technique applied uniformly. Each grade requires calibrated judgment — knowing how much glandular tissue to preserve to prevent a crater deformity, how to feather VASER margins for a natural transition, and how to position the circumareolar closure for a natural areola shape. A surgeon operating across all four grades regularly brings a different level of precision to each.
Dr. Pradeep Kumar Singh — MCh in Plastic Surgery, SMS Medical College, Jaipur; Fellowship in Advanced Aesthetic Surgery, St Louis Hospital, Paris; APSI member — performs male breast reduction surgery across all four Simon classification grades at Artemis Hospital, a JCI and NABH-accredited facility in Sector 51, Gurugram. His assessment process identifies grade, tissue composition, and skin status — and maps each finding directly to a surgical plan.
Patients from Palam Vihar, Nirvana Country, Sector 57, DLF Camelia, Golf Course Extension, Sohna Road, Vasant Kunj, South Extension, and Chanakyapuri travel to Artemis Hospital because the grade assessment is clinical and specific — not a general conversation about whether surgery is needed.
Frequently Asked Questions
How do I know if I have true gynecomastia or just chest fat?
Apply firm pressure directly behind the nipple. True gynecomastia produces a firm, rubbery disc that does not compress like fat. Pseudogynecomastia presents as soft, diffuse fullness without a firm central mass. Many cases are mixed. A clinical examination formally distinguishes the two and assesses the proportion of each, which determines the surgical approach.
Can Grade I or Grade II gynecomastia be treated without surgery?
In adolescents, a watch-and-wait period of twelve to eighteen months is reasonable, as spontaneous resolution is possible. In adult men, established glandular tissue is metabolically inert — it will not reduce with exercise, diet, or medication. Surgery is the only effective treatment for the glandular component.
Will gynecomastia surgery leave visible scars?
The periareolar incision sits at the natural areola border — one of the least conspicuous scar locations on the body. By three to four months, it has faded to a thin line not visible through clothing. Grade III surgery produces more extensive scarring, discussed explicitly during the consultation. Full scar maturation takes six to twelve months for all grades.
What is the difference between VASER gynecomastia and traditional liposuction for gynecomastia?
VASER liposuction uses ultrasound energy to emulsify fat before removal, producing smoother contouring and less bruising than mechanical suction alone. In gynecomastia surgery, VASER is preferred for the chest because smooth contour transitions are critical for a natural result. Neither VASER nor traditional liposuction removes glandular tissue, which requires direct excision regardless of the liposuction method used.
Know Your Grade. Choose the Right Surgery.
The four grades of gynecomastia require four different surgical approaches. The man who needs a 45-minute excision and the man who needs a subcutaneous mastectomy with skin excision describe the same problem, but they need different procedures and different recovery planning. The grade assessment is where that distinction is made clearly.
Book now or call +91 82879 23924 to schedule your gynecomastia grade assessment with Dr. Pradeep Kumar Singh.
Or visit Artemis Hospital, Sector 51, Gurugram, Haryana 122001.
Read patient reviews and learn more at Dr. Pradeep Kumar Singh on Google.
Dr. Pradeep Kumar Singh — MCh Plastic Surgery, Fellowship Paris, APSI Member — Artemis Hospital, Sector 51, Gurugram.